|
Fluorescein angiography (FA) is helpful in differentiating between the various causes of a localized macular neurosensory detachment of the retina. Central serous retinopathy is characterized by leakage from an incompetent RPE layer and can produce localized neurosensory detachments. Occasionally, the appearance of a pseudohypopyon can develop with layering of the subretinal fluid and lipofuscin 1 ( Fig. The presence of lipofuscin in the subretinal space produces a yellowish color that is seen with Best’s disease and pseudovitelliform macular dystrophy. Choroidal neovascularization and macroaneurysms are common causes of subretinal fluid, hemorrhage, and lipid ( Fig. Other materials, like lipid and lipofuscin, also collect in this position. Again, the most common substances that accumulate in this area are fluid and blood. The subretinal location is the next potential space internal to the RPE. These lesions most commonly are caused by age-related macular degeneration or other causes of choroidal neovascularization and can be present with central serous chorioretinopathy. 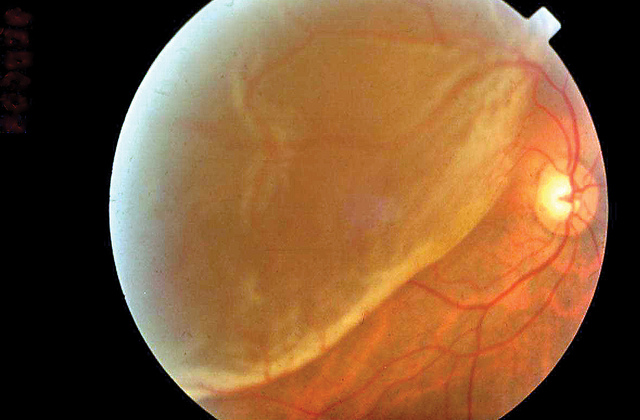
A fluorescein angiogram is instrumental in differentiating between the various types of PEDs. Other forms of PEDs develop from bleeding or large drusen formation beneath the RPE, termed hemorrhagic or drusenoid PEDs, respectively ( Fig. Transillumination of the lesion with a slit beam will often differentiate a serous and fibrovascular PED. A serous PED results from a collection of fluid beneath the RPE whereas an ingrowth of choroidal neovascularization is categorized as a fibrovascular PED. These elevated areas will often appear as a small, rounded, yellowish gray elevation of RPE underneath an otherwise normal retina. A change in this location will result in a pigment epithelial detachment (PED). The sub-RPE area is another location where pathology can occur and produce elevation of the macula. :max_bytes(150000):strip_icc()/retinal-detachment-3422079_final-63cc881b74d24520b72cc4691c8616f6.jpg)
Common causes of choroidal effusion include ocular hypotony, uveitis, and scleritis. 
Elevation of the choroid from suprachoroidal hemorrhage or thickening of the choroid due to choroidal effusions can secondarily elevate the macular retina and produce metamorphopsia ( Fig. Most of the changes at these levels are caused by abnormal accumulation of fluid, blood, or other substances, like lipofuscin. These include, from outer to inner layers, suprachoroidal space, choroid, subretinal pigment epithelial (RPE) space, subretinal space, and intraretinal space. This occurs when the normal concavity of the fovea is disrupted however, changes can occur in the macula that are extrafoveal and therefore do not affect the foveal light reflex.įive areas can be involved in producing an elevated or thickened macula. The most obvious sign of a thickened or elevated macular retina is often the loss of the foveal light reflex. A thorough fundus examination with biomicroscopy and utilization of a fundus contact lens is necessary to appreciate the subtle changes that may be present. How Do You Differentiate the Causes of Metamorphopsia?ĭetermining the morphology of the macula is crucial in determining the cause of metamorphopsia. A systematic approach to the evaluation of these symptoms is outlined in Figure 16–1. These symptoms can be unilateral or bilateral and are often asymptomatic when the pathology is unilateral with normal vision in the unaffected eye or when the fovea is uninvolved. Multiple symptoms are commonly experienced, including decreased vision (a decline in central visual acuity affecting distance and near vision), metamorphopsia (image distortion, the most sensitive symptom for macular elevation) ( Table 16–1), micropsia (objects appear smaller than normal), dyschromatopsia (colors appear faded), and loss of contrast sensitivity. Tell your eye doctor right away if you notice symptoms of vitreous detachment so they can check for these more serious problems.What Are the Symptoms of a Thickened or Elevated Macular Retina? These conditions can cause vision loss - but treatment may help preserve your vision. This usually happens slowly in the months or years after vitreous detachment. Sometimes vitreous detachment causes a thin layer of scar tissue to grow over the macula. This can happen before or after the vitreous detaches enough to cause floaters or flashes of light. Sometimes vitreous detachment tears a hole in the macula (the part of the retina that controls your central vision). 
Sometimes vitreous detachment pulls the entire retina away from its normal position at the back of the eye. If you don’t get treatment quickly, this can lead to retinal detachment. Sometimes, the vitreous fibers tear a hole in the retina when they pull away. Vitreous detachment can sometimes lead to more serious eye conditions:
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
